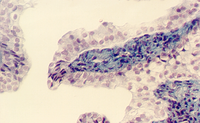
Kidney Glomerulus
If you hold the section of the kidney up to the light, you can distinguish the CORTEX from the MEDULLA. In the Masson stained section, note the blue-stained CAPSULE covering the surface. View the same regions with the low magnification of the microscope.

The outer regions, called the cortex are distinguished by numerous sectioned profiles of tubules and glomeruli. Identify the capsule and look at a glomerulus with a higher magnification. It is essentially a tuft of capillaries embedded in a double-walled epithelium (like a fist in a balloon). The epithelium is called "Bowman's capsule". That part of the epithelium covering the capillaries is called the visceral epithelium. The part forming the capsule is called "parietal epithelium". The filtration membrane is formed from the endothelial cells of the capillaries, basement membrane, and visceral epithelium. What cell types are found in the visceral epithelium? Draw the epithelial cell that forms the filtration membrane or barrier.
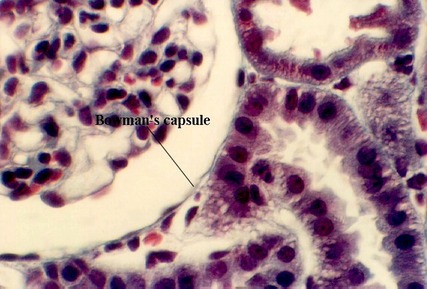
The above photograph shows a higher magnification of the glomerulus in Bowman's capsule. Note the capillaries in the glomerulus. The space between the two epithelia is called Bowman's space. Draw an arrow showing the route and direction of the urinary filtrate across the filtration membrane. Where does the filtrate go after it passes the filtration membrane?
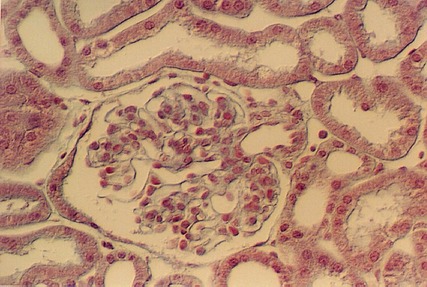
The above photograph is from Hematoxylin and Eosin stained kidney slide. Look at glomeruli in this slide and identify the capillaries, Bowman's capsule and Bowman's space. The afferent arteriole is the source of the capillaries in the Glomerulus. It is shown in this photograph, although the smooth muscle cells are difficult to see. The site where the arteriole enters the Renal corpuscle is called the "Vascular Pole". The opposite end is continuous with the proximal convoluted tubule. The above micrograph shows cells of the Proximal tubule beginning and joining with the cells of the Bowman's capsule (parietal epithelium). This is called the Urinary Pole. Find the vascular pole and the urinary pole on the above photo and following photographs. Also, find examples in your slide set.
.

The above photograph shows a higher magnification of the Urinary pole. It shows the transition between Bowman's Space in the Renal Corpuscle and the Proximal Convoluted tubule. Note that the cells show an abrupt transition from simple squamous to simple cuboidal in the proximal tubule (PT). Note also that the connective tissue elements supporting the tubules are stained bright blue in this Masson stained section.
Kidney Nephron
The nephron is the basic structural unit of the kidney. It is a tubule that consists of different regions which handle the glomerular filtrate conserving valuable salts, water, proteins. Each region is a simple epithelium that is specialized to handle the unique functions. It begins with the PROXIMAL CONVOLUTED TUBULE. These are very long and tortuous and remain in the cortex. Therefore, in a given section you will see more profiles of proximal tubules than the distal tubules.
The proximal tubule then changes to squamous epithelium which passes down to the medulla and then loops back up to the cortex. There are "highways" of tubules called "MEDULLARY RAYS" that contain tubules passing to the medulla. The thin part of the nephron is called the "LOOP of HENLE". As it ascends to the cortex again, it thickens to form the "THICK ASCENDING LIMB" of the Loop of Henle. Then, it becomes cuboidal and forms the DISTAL CONVOLUTED TUBULE. This part of the nephron joins with the COLLECTING TUBULES which then descend to the medulla in the medullary rays.
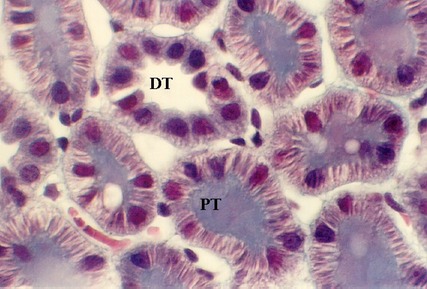
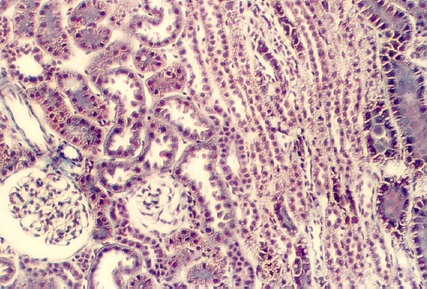
The profiles of the cortex will show proximal and distal tubules. They are supplied by a capillary network, called the Peritubular capillaries. In the above photograph, numerous proximal tubules are seen (PT). The cells are distinguished by an uneven apical border (because it is a brush border). Also, the base of the cells have many interdigitating processes that are filled with mitochondria. These can be visualized in the Masson stained section, shown above, as "ridges" running through the cells.
In contrast, Distal tubules have no brush border (DT). They have lateral interdigitations, however. They are distinguished from proximal tubules by the fact that they have a smoother apical surface. Also, the cells are smaller. Therefore, it is likely that one will see a nucleus in every profile. In contrast, proximal tubule cell profiles may not show as many nuclei. Find a peritubular capillary in the above photograph by the presence of stacked red blood cells.
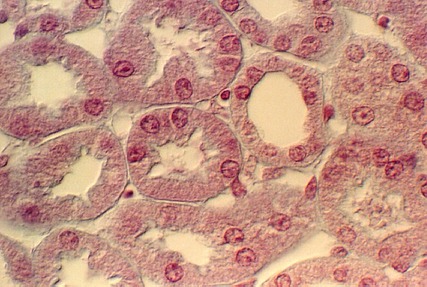
These photos are from the H & E stained section. Find a proximal tubule and a distal tubule in each of the photographs.
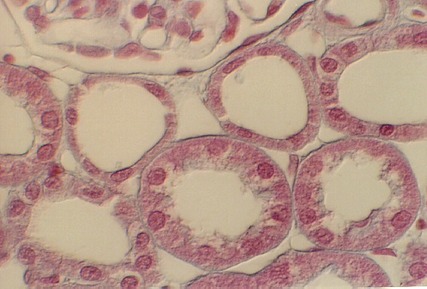
Understand the electron microscopic view of a proximal and a distal tubule cell
Understand the function of the Proximal and Distal tubules?

Find a medullary ray in your slides. In the rays, you can identify the LOOP OF HENLE by its squamous epithelium. Also, you can see COLLECTING TUBULES by their cuboidal epithelium. The vessels in the medullary ray are the VASA RECTA.

The above photograph shows an example of a Loop of Henle in a ray. Also, the vasa recta can be distinguished by their content of red blood cells. What is the function of the Loop of Henle?
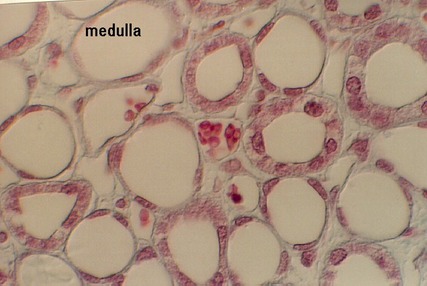
Move into the medulla and find the tubules there. You should be able to distinguish the VASA RECTA by their content of blood cells. Also, the thin limbs and the thicker limbs of the LOOP of HENLE can be seen. Finally, the COLLECTING TUBULES are cuboidal and columnar. They grow taller as they descend in the medulla. Identify the three types of tubules in the above photograph by the size and shape of their epithelium and the presence or absence of blood cells. What is the function of the thin limb of the Loop of Henle? What is the function of the Vasa recta? What is the function of the Collecting ducts?
Kidney Blood Supply
It is very important to have a complete understanding of the distribution of blood vessels to the kidney, considering its function. Review your lecture notes and text and follow the vessels as they penetrate the kidney, divide into branches and move to the cortex. What is the advantage of routing the blood to the cortex first, before it goes to the medulla?
Try to find some of the key arteries in your section, using the following guide. First, look at the border between the cortex and medulla and see if there are any vessels running perpendicular to the medullary rays. These are the ARCUATE ARTERIES that arch over the medulla and send arteries up to the cortex. The following photograph shows an arcuate artery. Admittedly it is difficult to tell in this view, because the medullary ray can't be seen. Your slides should allow you to find medullary rays, however.
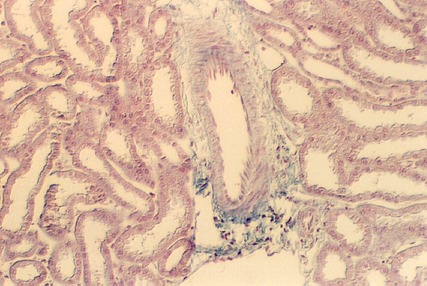
Move up into the cortex of your kidney slides and find medullary rays. Then find large arteries that run parallel to the rays. These are called the INTERLOBULAR ARTERIES . If you are lucky, you can also see some Interlobular arteries (IL A in following photo) that are branching and penetrating the lobules. These are the AFFERENT ARTERIOLEs and you may be able to follow them all the way to the glomerulus as is shown in the following photograph. Then, the afferent arterioles break up into the glomerular capillaries. These converge and form another arteriole that leaves the glomerulus called the EFFERENT ARTERIOLE.

The following photograph shows two arterioles supplying a glomerulus. You would not be able to distinguish the Afferent from the Efferent arterioles unless you could trace the former to a connection with the Interlobular artery.
The Efferent arterioles then break up into a second set of capillaries that surround the tubules in the cortex. These are called the PERITUBULAR CAPILLARIES. You found them in previous units on the cortex. Near the medulla, the Efferent arterioles also form vessels that loop down to the medulla, running in the medullary rays. These are the VASA RECTA. You identified them while you were studying the tubules of the nephron. Both the peritubular capillaries and the vasa recta join with arcuate veins which then follow the arterial path out to the renal vein.
After you identify as many of the vessels you can find (from the arcuate artery on), then write out or draw the pathway of the arterial supply to the kidney cortex. When you get to the capillaries or vasa recta, name the epithelia or tubules that are supplied by each of the vessels.
The JuxtaGlomerular Apparatus
After you have identified the vessels, you can better understand the organization of the endocrine system in the pituitary called the Juxtaglomerular apparatus (JG apparatus). This apparatus is found near each glomerulus where the afferent and efferent arterioles lie next to a distal tubule. The cells of the distal tubule become taller and form a structure known as the MACULA DENSA. Somehow this group of cells are specialized to sense the fluid volume and pass this information on to some specialized SMOOTH MUSCLE CELLS in the Afferent and Efferent Arterioles. These are called JUXTAGLOMERULAR CELLS. They have differentiated into endocrine cells and they produce a hormone (which is really an enzyme) called RENIN. Renin is produced on rough endoplasmic reticulum and packaged in large granules. Together, the Macula Densa and the JG cells are called the JG apparatus. Several views are seen in the photographs below.

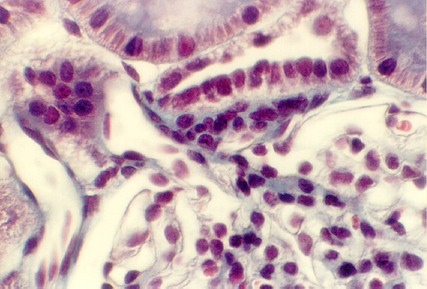
Note that the Macula cells in the distal tubule are taller.
Label the JG cells and the Macula densa in the above photograph.
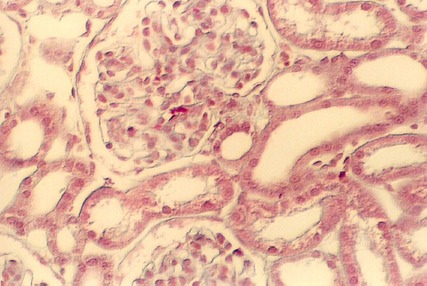
The above photo shows a JG apparatus in the H & E stained section. Label the JG apparatus.
After you have found this structure in your kidney slides, review the function of each part. What is the function of renin? List each step in the cascade leading to stimulation of the adrenal. What is the function of aldosterone? Draw a electron micrograph of renin producing cells (JG cells).
Calyces, Ureter & Bladder
The collecting ducts become taller as they descend in the medulla. Eventually they become the columnar DUCTS OF BELLINI. The epithelium then joins with that of cup like extensions of the ureter called the MINOR CALYCES (singular=calyx). The minor calyces are branches of the MAJOR CALYCES. The epithelium of the minor and major calyces is transitional, beginning with 2-3 layers and ending with 8 or more layers. You may find parts of the calyces on your kidney slides, especially the Masson stained slide.
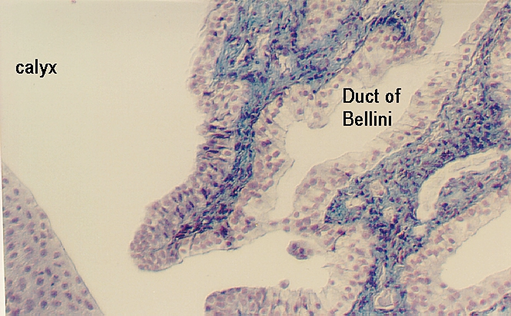
The above photograph shows the transition between the Duct of Bellini and the minor calyx. Note the increase in number of layers in the epithelium. Urine is emptied into the calyces which are like funnels that send it to each of the ureters. Note the extensive connective tissue that underlies the epithelium in this region (stained blue). The following photo shows a higher magnification of the transitional region. Some areas still have only a simple columnar epithelium, others have the mixture of types of epithelia typical of transitional epithelium.
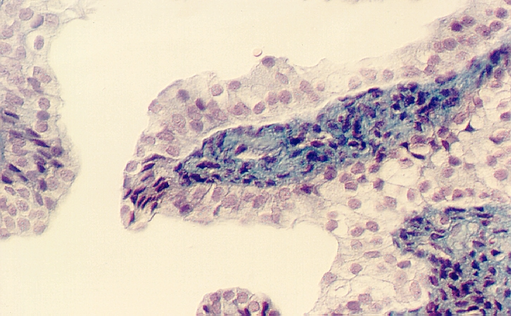
The major calyx may be distinguished by its number of layers of cells.
The following photograph shows the wall of a major calyx. Again, the
epithelium is transitional, like that of the ureter.

After they begin in the calyces, the two muscular tubes, the URETERS, conduct the urine to the bladder. The following photograph shows the transitional epithelium in the ureter. Find it in your ureter slide. Recall that it is distinguished by rounded cells at the surface. It is a mixture of columnar and cuboidal epithelia which is how it got its name.
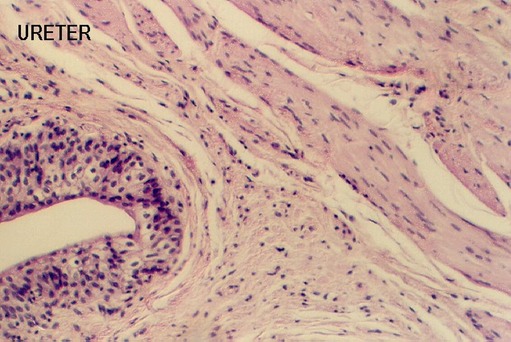
Underneath the epithelium is a layer of connective tissue. Then, there are three layers of smooth muscle. The innermost is longitudinal (cut in cross section in your sections), the middle is circularly arranged around the tube (cut in longitudinal section) and the outer is longitudinal again. Look at the muscle in your ureter slide and find a region that shows the three layers distinctly. The following photo illustrates such a region.

The above photograph shows the inner, middle, and outer smooth muscle
layers of the ureter. Outside the muscle wall is the ADVENTITIA which is loose connective
tissue. Draw the ureter and show how it ends in the major and minor calyces in the
kidney.
The urinary bladder is relatively simple in that it has a transitional epithelium, an underlying connective tissue (LAMINA PROPRIA) and an interwoven smooth muscle wall which shows no distinct layers (MUSCULARIS). Outside the muscular wall is the connective tissue ADVENTITIA. Find these regions in your bladder slide. These photos show the bladder epithelium. Note the rounded bulging cells facing the lumen. Also, note the underlying lamina propria in the above photo.
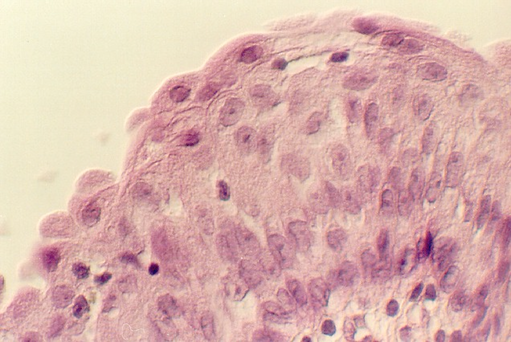
What structures enable the transitional epithelium to distend? Consult an electron microscopic view of the epithelial cells.
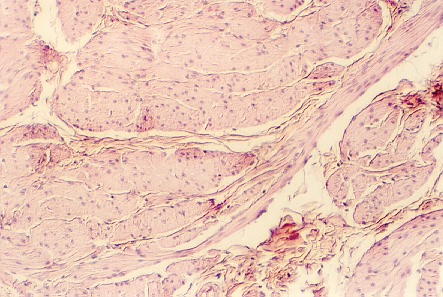
Note the interlacing muscle bundles in the wall of the bladder, separated by connective tissue as shown in the above photo. There are no organized layers of smooth muscle in the wall.
http://microanatomy.net/kidney/kidney.htm
Gwen V. Childs, Ph.D., FAAA
Department of Neurobiology and Developmental Sciences
University of Arkansas for Medical Sciences
4301 W. Markham, Slot 510, Little Rock, AR 72205
For questions or concerns, send email to this address